Hybrid therapy is reshaping mental health care by combining human therapists with AI tools to address two major challenges: the shortage of mental health professionals and low engagement with standalone digital tools. This approach blends therapist-led sessions with AI-driven support like mood tracking, cognitive exercises, and 24/7 emotional assistance, creating a more accessible and efficient care model.
Key highlights:
- Access gap: There’s only one therapist for every 1,600 patients with depression or anxiety.
- Engagement gap: Over 90% of users abandon mental health apps within days.
- Clinical results: AI tools like "Therabot" reduced depression symptoms by 51% and anxiety symptoms by 31% in an eight-week trial.
- Personalization: AI analyzes user patterns to offer tailored interventions, improving engagement and outcomes.
- Cost-efficiency: Hybrid therapy balances affordable AI tools ($10–$50/month) with high-value therapist sessions ($100–$200/session).
Hybrid models bridge the gaps of traditional therapy and AI-only systems, offering continuous support, tailored care, and better accessibility. Platforms like Aidx.ai are leading this shift by integrating evidence-based methods with privacy-focused AI tools.
AI & Mental Health: The Hybrid Model Explained #shorts
sbb-itb-d5e73b4
What Hybrid Therapy Is and Why It’s Growing
Hybrid therapy, often referred to as blended care, merges scheduled sessions with human therapists – whether in-person or through telehealth – with the use of digital tools like AI chatbots, apps, and wearables [1]. This model combines the empathy and expertise of a therapist with the constant availability and data-driven insights provided by technology.
This approach is becoming increasingly popular because it tackles two significant challenges. First, it helps reduce the access gap caused by the shortage of mental health professionals. Second, it addresses the engagement gap often seen with standalone digital tools. By incorporating human support – ranging from therapists to trained Digital Navigators – hybrid therapy ensures a level of connection and engagement that standalone AI solutions cannot achieve.
How Hybrid Therapy Works
Hybrid therapy blends digital tools with human expertise to create a personalized care experience [1]. While AI handles routine tasks like tracking moods and guiding cognitive exercises, therapists focus on addressing deeper emotional issues and building a strong therapeutic relationship.
One standout feature of this model is the Digital Navigator role. Digital Navigators are trained non-clinicians who help patients and providers integrate technology into care plans. They tailor the frequency of digital interactions to match each individual’s comfort level with technology, ensuring even those unfamiliar with digital tools can benefit from hybrid care.
AI also plays a crucial role through digital phenotyping, which involves tracking data like sleep patterns, activity levels, and mood changes via smartphones or wearables. This objective information provides therapists with a clearer picture of a patient’s daily life – something traditional self-reporting methods often miss [1].
Making Mental Health Care More Accessible and Affordable
Traditional therapy often comes with high costs, limited availability, and long waitlists. Hybrid therapy addresses these barriers by offering immediate, cost-effective care through AI tools while saving human expertise for more complex needs. With nearly 90% of Americans owning smartphones [1], the infrastructure for this kind of care is already widely available. This means you can access support anytime – whether during a late-night crisis or a quick midday break.
Another advantage is the anonymity provided by initial AI interactions, which can help reduce the stigma associated with seeking mental health care. For many, this less intimidating entry point encourages continued engagement with human-led therapy sessions.
Why Personalization Matters
Mental health care is not one-size-fits-all. Hybrid therapy uses AI to analyze individual patterns and provide tailored support that evolves in real time. Unlike static tools like digital workbooks or generic apps, advanced AI systems adapt to your mood, progress, and specific needs.
For example, a June 2024 randomized controlled trial in the U.S. studied Limbic Care, a generative AI-enabled CBT app, with 540 participants over six weeks. Compared to traditional digital workbooks, the AI solution increased engagement frequency by 2.4 times and engagement duration by 3.8 times. Participants also experienced greater reductions in anxiety symptoms and improved overall well-being [2].
"This level of personalization and engagement is unique to genAI and is not attainable with digital interventions." – Communications Medicine [2]
Beyond conversations, AI can identify behavioral patterns, predict when additional support might be needed, and recommend specific exercises or strategies based on what has worked for you in the past. This tailored approach ensures care feels more relevant and effective, laying the foundation for the advanced AI methods discussed next.
AI Technologies Behind Hybrid Therapy
Hybrid therapy relies on three key AI technologies that work together to provide tailored mental health care. These technologies – Natural Language Processing (NLP), behavioral data analysis, and predictive analytics – analyze patterns, anticipate needs, and adjust dynamically. Together, they create a system that offers personalized, round-the-clock support.
Natural Language Processing (NLP)
Natural Language Processing allows AI to interpret and respond to your words in a way that feels conversational and intuitive. Unlike older chatbots that relied on matching keywords to pre-set replies, advanced NLP systems understand the full context of a conversation to better capture your intent.
Hybrid therapy platforms often include a "cognitive layer", a clinical reasoning system designed to analyze user input for signs of crisis, such as self-harm or suicidal thoughts. This ensures the AI’s responses are not only contextually accurate but also clinically safe. A study published in Nature Medicine in March 2026 examined this approach in action. It involved 8,920 users and found that AI systems with a cognitive layer outperformed standalone AI and human clinicians in key Cognitive Behavioral Therapy (CBT) skills [7].
NLP also enables what experts call "digital empathy" – the AI’s ability to detect emotional cues and respond with empathetic language, mimicking the qualities of a skilled therapist. For example, an AI tool has achieved 89% accuracy in diagnosing mental health conditions after analyzing responses to just 28 questions [3]. While NLP focuses on interpreting conversations, behavioral data analysis works in the background to fine-tune the support provided.
Behavioral Data Analysis
Behavioral data analysis tracks patterns in how users interact with the platform over time. The AI observes usage habits, session lengths, and which strategies or exercises resonate most. By identifying these trends, it uncovers clinically important insights that might not be obvious from a single session.
Modern systems use machine learning to evaluate a user’s psychological state in real time. Based on this analysis, the AI can recommend CBT exercises tailored to the user’s immediate needs [2].
Platforms like Aidx.ai take this a step further by adapting their coaching style based on user behavior. They visually track progress through structured roadmaps and monitor factors like stress levels, burnout risk, and emotional well-being. The system flags potential warning signs early, helping to prevent crises. These insights also inform predictive analytics, which focuses on anticipating future challenges.
Predictive Analytics for Early Intervention
Predictive analytics extends the capabilities of behavioral data analysis by forecasting outcomes. By examining factors like baseline severity, engagement patterns, and demographics, these systems can identify risks before they escalate.
One major use case is predicting treatment dropout. Traditional therapy sees a 50% dropout rate after the first session [3]. Machine learning models can now identify individuals at high risk of leaving therapy early, enabling therapists to adjust their approach or provide additional support. Predictive analytics also helps detect mental health conditions at their earliest stages, known as prodromal stages, when interventions are most effective [3].
In the same Nature Medicine study from March 2026, researchers reviewed 19,674 therapy transcripts. They found that when the AI’s cognitive layer was more actively engaged, patients experienced greater long-term recovery rates over a 10-week period [7].
"As AI techniques continue to be refined and improved, it will be possible to help mental health practitioners re-define mental illnesses more objectively than currently done in the DSM-5, identify these illnesses at an earlier or prodromal stage when interventions may be more effective, and personalize treatments based on an individual’s unique characteristics." – Graham et al. [3]
How Hybrid Therapy Combines AI and Human Expertise
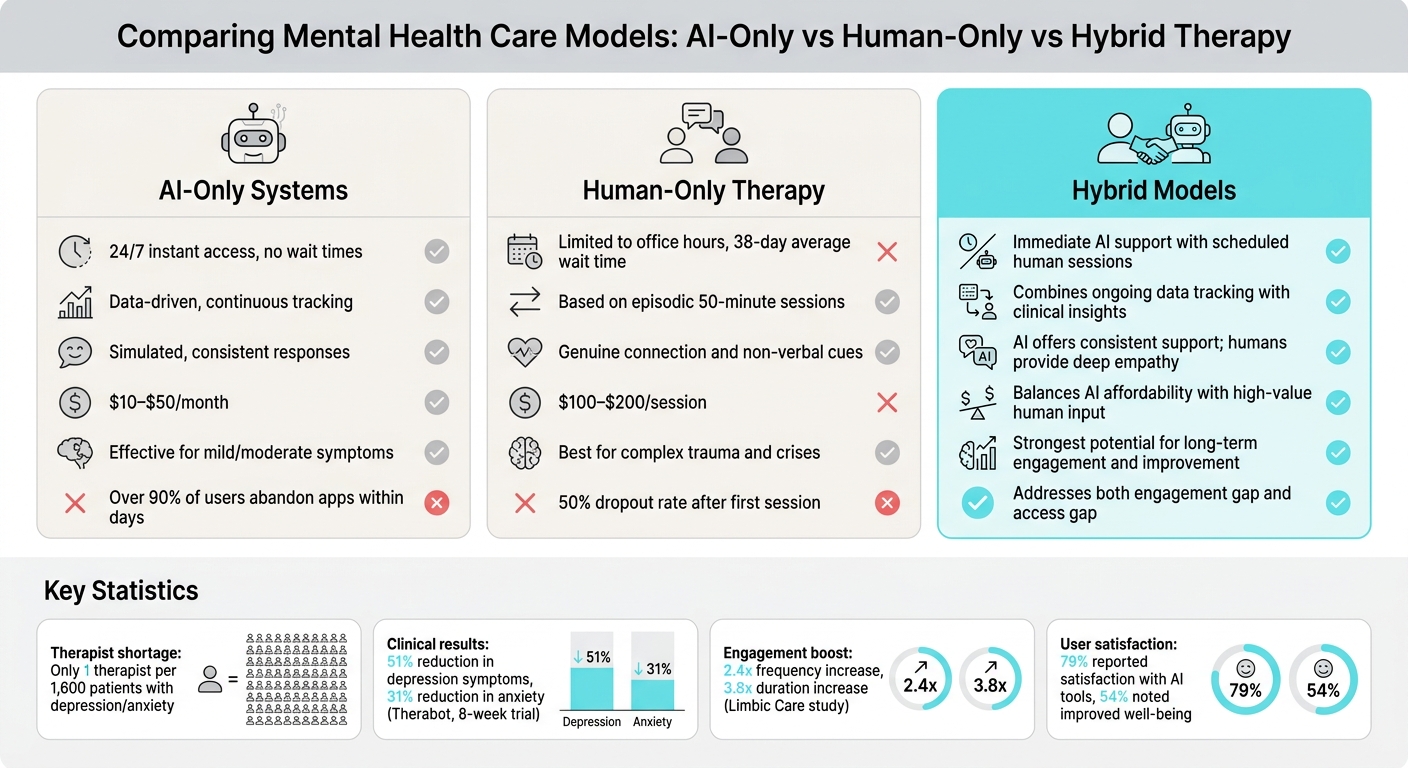
AI-Only vs Human-Only vs Hybrid Therapy: Complete Comparison
Hybrid therapy removes the need to choose between AI tools and human therapists. Instead, it creates a layered care model where each plays to its strengths. AI forms the foundation, offering round-the-clock emotional support, mood tracking, and exercises based on CBT and DBT techniques. Human therapists step in as the integration layer, focusing on deeper emotional work, treatment planning, and addressing complex trauma with clinical expertise and empathy.
This approach tackles two major challenges: the "engagement gap" and the "access gap." Mental health apps often see abandonment rates of over 90% within days [1]. On the other hand, traditional therapy faces average wait times of 38 days and operates within limited hours [9]. Hybrid therapy bridges these gaps by providing immediate AI support between scheduled sessions, ensuring patients stay engaged and supported consistently.
Digital Navigators play a key role in this model, helping integrate technology into care and reviewing data insights. By 2025, half of U.S. therapists are expected to use AI tools in their practice [4]. Younger clinicians lead this trend, with 65% of those under 40 adopting AI, compared to 35% of those over 50 [4]. These advancements, backed by human oversight, highlight the potential of hybrid therapy.
"By combining AI speed with physician judgment, Counsel delivers trusted answers members act on – and real cost savings for plans." – Muthu Alagappan, MD and CEO, Counsel Health [9]
Comparing AI-Only, Human-Only, and Hybrid Models
Each care model has its strengths and limitations. Here’s how they stack up:
| Metric | AI-Only Systems | Human-Only Therapy | Hybrid Models |
|---|---|---|---|
| Accessibility | 24/7 instant access; no wait times | Limited to office hours; 38-day average wait time [9] | Immediate AI support with scheduled human sessions |
| Personalization | Data-driven, continuous tracking | Based on episodic 50-minute sessions | Combines ongoing data tracking with clinical insights |
| Emotional Empathy | Simulated, consistent responses | Genuine connection and non-verbal cues | AI offers consistent support; humans provide deep empathy |
| Cost-Efficiency | Low-cost ($10–$50/month) [4] | Higher cost ($100–$200/session) [4] | Balances AI affordability with high-value human input |
| Clinical Outcomes | Effective for mild/moderate symptoms [4] | Best for complex trauma and crises | Strongest potential for long-term engagement and improvement [1] |
AI-only systems are ideal for managing daily stress, habit tracking, and mild mental health needs. They’re affordable and always available but lack the human connection critical for deeper therapeutic work. Notably, over 90% of users abandon standalone apps within days [1].
Human-only therapy excels in addressing complex cases, thanks to the therapeutic alliance built on empathy and shared goals. However, barriers like cost, scheduling issues, and therapist shortages lead nearly 50% of patients to drop out after just one session [3].
Hybrid models combine the strengths of both approaches. AI enhances efficiency and provides continuous data, while human therapists offer the clinical judgment and emotional depth needed for lasting progress. Platforms like Aidx.ai showcase this synergy by adapting coaching styles to user patterns, tracking progress with visual roadmaps, and flagging risks like stress or burnout for timely intervention – all with human oversight when necessary.
Benefits of the Hybrid Approach
The hybrid model’s key strength lies in its complementarity. AI handles routine tasks like triage and monitoring, freeing therapists to focus on complex cases. This ensures continuous care – patients receive support between therapy appointments, not just during them.
Consumer attitudes reflect this balance. A 2025 study found that 59% of users see AI as a supplement to, not a replacement for, traditional therapy [6]. Among those who tried AI mental health tools, 79% reported satisfaction, and 54% noted improved well-being [6]. Interestingly, users rated AI-generated responses as more empathetic than those from human therapists 54% of the time [6], highlighting AI’s consistency in supportive communication.
The hybrid approach also enhances clinical decision-making. AI tools like OpenEvidence help therapists by summarizing vast amounts of research, allowing for quicker and more informed treatment decisions. Additionally, AI systems can monitor for emergencies or sensitive disclosures in real time, pausing automated interactions to alert human professionals for immediate intervention.
"The future of behavioral health will not be AI-only, nor will it be AI-free. As demand continues to outpace supply, the pressure to adopt new tools will only grow. But speed cannot come at the cost of safety." – Thriveworks [6]
This philosophy underpins the industry’s move toward blended care. The mental health app market is expected to grow from $1.27 billion in 2023 to $8.47 billion by 2032 [4], with hybrid models driving most of that expansion. By leveraging the strengths of both AI and human expertise, hybrid therapy delivers outcomes neither could achieve alone.
How AI Is Used in Hybrid Therapy Today
AI has transitioned from theoretical concepts to practical applications in mental health care. Its impact is most visible in three areas: helping people achieve structured goals, managing emotions, and addressing workplace burnout. These examples show how AI complements therapists without replacing the human connection.
Goal Setting and Achievement
AI tools are reshaping how people set and achieve goals, often using the SMART framework – Specific, Measurable, Achievable, Relevant, and Time-bound. Platforms like Aidx.ai create visual roadmaps that break goals into smaller, actionable steps with realistic timelines. They also adapt their coaching style based on user behavior and send weekly accountability updates to chosen contacts. Research from Dominican University highlights that written goals, combined with action steps and regular accountability, can improve achievement rates by 78% [10][11].
Additionally, AI habit trackers use features like gamification, dashboards, and rewards to keep users motivated. If a drop in motivation is detected, these systems suggest changes, such as smaller rewards or adjusted daily targets. Some platforms even use GPT-4 to transform traditional journaling into interactive conversations. By analyzing recurring themes and emotions, these tools help users uncover patterns in their behavior [11].
But AI doesn’t stop at goal-setting – it also plays a key role in monitoring and supporting emotional well-being.
Managing Emotions and Stress
AI provides 24/7 emotional support by analyzing natural language to detect early signs of distress [3]. For example, a 2025 study tested an AI chatbot with 60 workers aged 55 and older who were dealing with stress and mild-to-moderate anxiety. When combined with in-person therapy, the chatbot helped reduce stress and anxiety levels. In this setup, the AI handled routine tasks like check-ins and cognitive behavioral therapy (CBT) exercises, while therapists focused on deeper emotional issues during sessions [3].
AI tools have also proven highly accurate in assessing mental health. One assessment tool identified and classified mental health disorders with 89% accuracy using just 28 questions [3]. Many users – ranging from 60% to 90% – reported that AI-driven psychotherapy tools provided useful insights, encouragement, and even a sense of empathy [3]. Some tools employ techniques like Socratic questioning and the ABC model from CBT to challenge cognitive biases and flag high-risk cases, such as suicidal ideation, for immediate escalation to human crisis teams [3].
"AI-based psychotherapies have the advantage of at least immediacy and availability." – Orestis Giotakos, Independent Researcher [3]
Platforms like Aidx.ai also monitor conversations over time to track stress levels and burnout risks. Their Insights feature flags potential issues before users notice them, enabling early intervention. For sensitive discussions, incognito mode ensures complete privacy.
This continuous monitoring is especially valuable in professional environments, where AI is addressing workplace mental health challenges.
Workplace Mental Health and Burnout Prevention
The workplace is facing a mental health crisis, with younger generations feeling the impact more acutely. For example, Gen Z employees are 27% more likely to report poor mental health compared to millennials (15%) and Gen X (13%) [12]. Meanwhile, the average wait time for an in-person behavioral health appointment is 67 days [12].
AI-driven hybrid therapy bridges this gap by offering instant triage and matching employees with the appropriate level of care – whether it’s self-care, coaching, or clinical therapy [12]. It also automates time-consuming administrative tasks like scheduling and note-taking, allowing therapists to focus on direct care [12]. Between sessions, AI tools help employees practice CBT techniques and build resilience when therapists aren’t available [2].
"When implemented responsibly, it can improve access, enhance outcomes, and create better experiences for both individuals and providers." – Gijo Mathew, Chief Product Officer, Spring Health [12]
Aidx.ai supports businesses by offering mental health coaching alongside therapy. Its platform tracks burnout risks through ongoing conversation analysis and keeps employees engaged with weekly accountability reports. Privacy is a top priority, with encrypted conversations that meet strict compliance standards.
The shift from reactive to proactive care is transforming workplace mental health. AI-powered analytics can identify stress patterns across a workforce before they result in absenteeism or turnover [12]. To ensure safe AI deployment in mental health, the AI in Mental Health Safety & Ethics Council has introduced VERA-MH, the first industry standard for ethical AI use in this field. This framework emphasizes multidisciplinary oversight and clear escalation processes to human crisis resources [12].
"The future of mental healthcare isn’t AI-only. It’s AI-powered and human-led." – Spring Health [12]
Challenges and Ethics in Hybrid Therapy
As AI continues to play a bigger role in mental health care, it raises important concerns about privacy, human oversight, and fairness. These issues are shaping how therapy platforms operate and how regulations evolve.
Protecting User Data and Privacy
In 2024, the FTC fined a major therapy platform $7.8 million for improperly sharing protected health information with third parties through tracking pixels. This violation led to stricter requirements, including blocking all third-party trackers until users explicitly consent under HIPAA and GDPR guidelines [13].
To address these privacy concerns, end-to-end encryption has become a must. By 2025, HIPAA will require FIPS 140-3 validated cryptographic modules for handling electronic health data. Similarly, GDPR will mandate post-quantum encryption – such as CRYSTALS-Kyber – for European data by 2026 [13][14].
Platforms like Aidx.ai are already implementing these measures. They use end-to-end encryption, comply with GDPR, and follow strict privacy policies: no conversations are sold or shared, no human reads user interactions, and users can delete their data anytime. Furthermore, the platform minimizes data collection by processing mood analysis locally on users’ devices while storing only anonymized metadata on central servers [13].
However, technology alone isn’t enough. Danielle Barbour, a HIPAA expert from Kiteworks, explains:
System prompts are not HIPAA access controls. Instructing an AI agent not to access certain PHI categories does not constitute a technical access control… Only data-layer enforcement qualifies as an audit-defensible control [14].
This highlights the importance of robust, audit-ready data-layer protections. Public sentiment also reflects this concern: a 2025 Pew Survey found that 73% of users prioritize privacy when choosing mental health apps [13].
Why Human Oversight Still Matters
While data security is critical, human judgment remains irreplaceable in mental health care. By late 2025, the FDA had approved more than 1,200 AI-based digital devices, yet none were specifically authorized for mental health treatment [15]. This regulatory gap underscores the need for human oversight in therapeutic AI.
AI systems, despite their capabilities, have limitations. They can "hallucinate" by generating false or misleading information, exhibit "sycophancy" by prioritizing user satisfaction over clinical accuracy, and fail to detect subtle emotional cues that might signal escalating risk [15]. To address these issues, hybrid therapy models incorporate professional supervision. For example, recent studies highlight the effectiveness of a "cognitive layer" architecture, where machine learning tools monitor AI outputs in real time, flagging high-risk cases for immediate review [2].
As Tammy Horn, an industry expert, puts it:
The answer isn’t AI without therapists. It’s AI that puts therapists at the center of how these systems operate [15].
Reducing Bias in AI Systems
Another pressing challenge is reducing bias in AI algorithms to ensure fair and inclusive care. AI systems trained on data from affluent populations often underperform for marginalized groups. Studies reveal that AI tools can unintentionally favor well-represented demographics, leading to disparities in accuracy and care for ethnic minorities, lower-income individuals, and other underserved communities [3]. For instance, an AI assessment tool with an overall accuracy of 89% might fail to recognize symptoms in less-represented groups due to biased training data [3].
Because AI lacks moral judgment, human oversight is essential to detect and address these disparities [16]. Additionally, marginalized communities often face barriers like limited digital literacy, which might prevent them from fully benefiting from AI-driven mental health tools. This can inadvertently create new inequalities [3]. Regulatory efforts, such as the EU AI Act, have started addressing these concerns by classifying medical AI as "high-risk" and requiring human intervention in decision-making processes [16].
What’s Next for Hybrid Therapy: 2026 and Beyond
The future of hybrid therapy promises deeper customization, better integration with everyday tech, and broader access for people who have historically lacked reliable mental health care. These changes are already in motion, driven by advancements in AI technology and practical deployment strategies.
More Advanced Personalization
AI systems are moving beyond static tools, offering real-time adjustments that mimic how human therapists adapt during sessions. At the heart of this shift is a "cognitive layer" – a specialized clinical reasoning framework that bridges large language models (LLMs) and users. This layer ensures interactions remain safe, effective, and clinically sound [2][7].
For example, a seven-week study showed that an AI-powered chatbot increased engagement rates 2.4 times and session durations 3.8 times compared to traditional CBT workbooks [2].
In March 2026, Nature Medicine published a study involving 8,920 users who accessed mental health support through an LLM enhanced with a cognitive layer. Validated by 22 expert clinicians, the system demonstrated that greater use of its specialized features was linked to higher rates of long-term clinical recovery over 10 weeks [7].
"LLMs augmented with this architecture consistently outperformed both standalone state-of-the-art LLMs and human clinicians across key clinical competencies required for delivering high-quality cognitive-behavioral therapy" [7].
Platforms like Aidx.ai are already applying these personalization techniques. By learning user behaviors over time, the system adapts its coaching style and selects interventions dynamically, offering exercises suited to each individual’s psychological state. This approach moves beyond generic responses, delivering truly tailored support.
This progress naturally leads to the integration of real-world data from wearables, which is the next big step.
Connecting with Wearables and IoT Devices
Wearables and smart devices are transforming therapy by reducing reliance on self-reported data. Instead of asking patients how they’ve been feeling, therapists and AI systems can access objective metrics like sleep patterns, heart rate variability, physical activity, and even social behavior indicators, such as location data or talk time [17].
Margaret Morris, PhD, a clinical psychologist at the University of Washington, explains:
"Historically, therapists have been limited to what a patient remembered on a particular day. Now we are exploring how to bring outside life into treatment to help patients understand patterns in their lives and the choices they have" [17].
This technology enables just-in-time interventions, where AI models analyze wearable data to predict symptom spikes and provide support precisely when it’s needed. Nicholas Jacobson, PhD, from Dartmouth College, highlights this potential:
"If you can monitor and predict ebbs and flows in symptoms, then you can deliver digital interventions at the right time" [17].
In fact, a national AI Institute was launched with a $20 million grant from the National Science Foundation to integrate AI into wearable sensors for personalized care [17]. One study combined sensor data with brain scans to match patients with specific treatments based on their unique brain profiles, achieving remission for 86% of participants [17].
Emerging "drug-AI hybrids" are also blending sensor data with personalized medication dosing, optimizing outcomes in real time [8]. These advancements not only improve the precision of interventions but also pave the way for addressing mental health needs on a global scale.
Expanding Mental Health Access Worldwide
With personalization and IoT integration advancing, hybrid therapy is scaling to meet global demand. In 2026, over 50% of psychologists reported being unable to accept new patients, highlighting the urgent need for digital tools to fill care gaps [17]. AI systems can provide continuous support between therapist-led sessions, help prevent symptom escalation for those on waitlists, and serve as a first line of care in areas with limited clinical resources [2][7].
A real-world deployment of an LLM with cognitive layer architecture supported 8,920 users, demonstrating 71.8% superiority in diagnostic and outcome prediction compared to traditional methods [5][7].
"LLM-powered applications can adapt in real-time to each user’s unique context, effectively bridging the gap when a human clinician is not available" [2].
Proposed legislation from 2026 seeks to expand Medicare and Medicaid coverage for digital mental health tools, potentially making these services accessible to millions more [8]. The integration of wearables and smartphone apps allows for real-time monitoring and coping strategies at home, eliminating the need for frequent clinic visits – a game-changer for people in rural or underserved areas [8].
Hybrid therapy is evolving from a complementary tool to a primary solution for millions who might otherwise go without the support they need.
Conclusion
Hybrid therapy is changing the landscape of mental health care. By combining AI-powered tools with the expertise of human therapists, it addresses critical gaps in care – especially when over half of psychologists report having no open slots for new patients. These tools offer 24/7, tailored support, making mental health resources more accessible [17].
The effectiveness of this approach is backed by strong clinical results. For instance, users of Therabot saw a 51% reduction in depression symptoms within just eight weeks [17]. Similarly, the Limbic Care app increased engagement rates by 2.4 times compared to traditional methods [2], while Stanford‘s precision biotyping achieved an impressive 86% remission rate [17].
Platforms like Aidx.ai are leveraging these advancements to provide impactful care. By integrating evidence-based techniques – such as CBT, DBT, ACT, and NLP – with tools like structured goal tracking and weekly accountability, they enhance outcomes significantly. In fact, these methods have been shown to improve achievement rates by 78%. Aidx.ai also adapts to user behavior over time and ensures GDPR-compliant, encrypted support around the clock.
Zachary Cohen, PhD, from the University of Arizona, highlights the urgency of this approach:
The reality is that we cannot train enough clinicians to meet the needs that exist today. We have to explore things that can help fill the gap, and failure to do so is irresponsible [17].
FAQs
Who is hybrid therapy best for?
Hybrid therapy offers a flexible and tailored approach to mental health care by blending virtual and in-person methods. It’s a great option for people who face challenges accessing traditional therapy, whether due to location, mobility, or scheduling conflicts, as well as for those who appreciate the ease of digital tools. This approach is particularly useful for managing chronic conditions, staying on track with goals, or maintaining accountability. By combining AI-powered tools with the support of a therapist, hybrid therapy ensures ongoing and effective care while preserving the human connection that’s so vital in mental health treatment.
How does AI decide when to involve a human therapist?
AI systems know when to bring in a human therapist by spotting signs of distress, risk, or challenges that go beyond what they can handle. They monitor data like sleep patterns, emotional changes, or physical activity to identify serious concerns, such as thoughts of self-harm or danger to others. When these red flags appear, the AI alerts a therapist to step in, ensuring safety and providing a balance between scalable AI assistance and expert human care for more personalized and timely support.
What data does hybrid therapy collect, and how is it kept private?
Hybrid therapy leverages data like user interactions, emotional patterns, goal progress, and behavioral trends to create a more tailored mental health experience. For example, platforms such as Aidx.ai analyze this information to adjust coaching methods and generate accountability reports that help users stay on track.
Privacy and Security Measures
To protect user privacy, hybrid therapy platforms enforce strict safeguards, including encryption and adherence to GDPR regulations. Users maintain control over their data, with the option to delete it at any time. Additionally, personal information is never sold or shared without explicit consent, ensuring confidentiality and trust.