Rural America faces a mental health care crisis. Over 65% of rural counties in the U.S. lack a psychiatrist, and 47% have no psychologist. On top of this, geographic isolation, limited public transit, and stigma make accessing care even harder. Personalized AI therapy and mobile health apps are changing this. These tools provide discreet, 24/7 access to evidence-based therapies like Cognitive Behavioral Therapy (CBT), helping users manage anxiety and depression from their homes.
Key takeaways:
- Provider shortages: Many rural areas have no mental health professionals.
- Barriers to care: 10% of rural residents live over 30 minutes from the nearest clinic.
- Mobile solutions: Apps like Aurora have shown measurable improvements in anxiety and depression symptoms.
- High interest: 97% of rural patients would use a prescribed digital therapeutic if recommended by a provider.
While these apps show promise, challenges like broadband access and long-term user retention remain. Addressing these issues can help bridge the rural mental health gap.
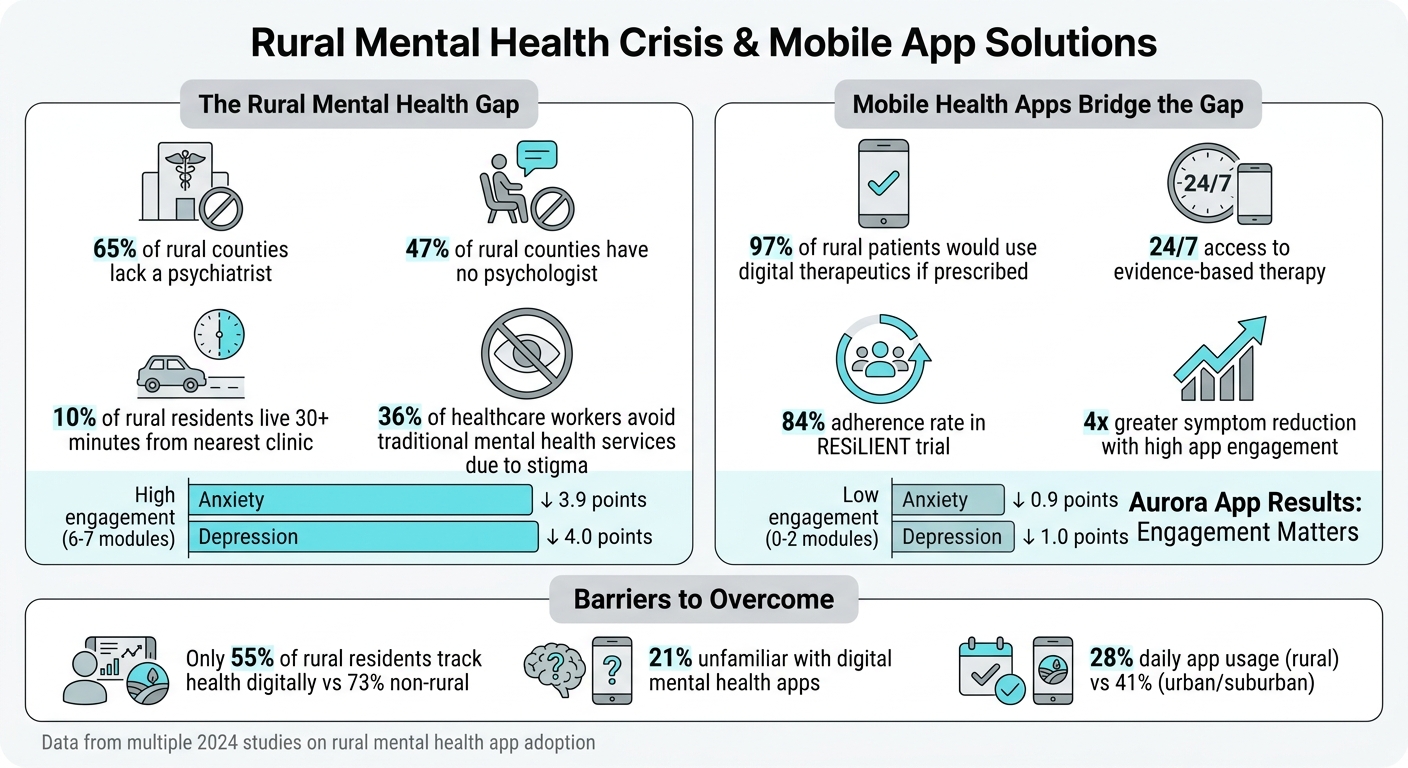
Rural Mental Health Crisis: Key Statistics and Mobile App Impact
How Smartphone Apps Can Improve Your Mental Health | Mass General Brigham
sbb-itb-d5e73b4
How Mobile Health Apps Expand Mental Health Access
Mobile apps are reshaping mental health care in rural areas by tackling key challenges like distance, cost, and stigma. They combine clinically proven features with affordable care, making mental health support more accessible than ever.
Overcoming Geographic and Infrastructure Barriers
For rural residents, access to mental health care often feels out of reach. Mobile apps change that by eliminating the need for travel and sidestepping infrastructure limitations. Consider this: 10% of rural Americans live over 30 minutes from the nearest medical facility [2]. For those without reliable transportation or public transit options, this can be a deal-breaker. Mobile apps, however, bring care directly to users, anytime and anywhere.
The shortage of mental health professionals in rural areas is another hurdle. 65% of rural counties lack even one psychiatrist, and 47% have no psychologist [2]. Mobile apps address this gap by offering 24/7 access to evidence-based treatments, removing the need for appointments, waiting rooms, or commutes [3].
Privacy is often a concern in small communities where anonymity is hard to maintain. Fear of being seen at a mental health clinic can deter individuals from seeking help. In fact, 36% of healthcare workers avoid traditional mental health services due to concerns about their reputation or professional consequences [3]. Mobile apps provide a solution by allowing users to seek treatment discreetly from the comfort of their homes, reducing the stigma that often prevents rural residents from accessing care [2][3].
Evidence-Based Therapeutic Features
Unlike generic digital content, mobile health apps are built on clinically validated interventions. Many apps include Cognitive Behavioral Therapy (CBT), which is widely recognized as an effective treatment for anxiety and depression. CBT helps users identify and change negative thought patterns while encouraging positive behaviors [1][4].
For example, the Aurora app demonstrated significant improvements in anxiety and depression symptoms among users who completed its eight-module CBT program [1]. Those who engaged more deeply – finishing six or seven modules – experienced symptom reductions four times greater than those who barely used the app [1].
Beyond CBT, apps often feature mindfulness exercises, problem-solving techniques, and therapies for insomnia [4]. Some even incorporate AI-driven chatbots, offering real-time emotional support and early detection of distress – an invaluable feature in areas with limited mental health specialists [3]. The RESiLIENT trial in Japan, which ran from September 2022 to February 2024, tested five CBT techniques through a smartphone app with 3,936 participants. The study achieved an 84% adherence rate, far surpassing the typical 30% for unguided internet programs, and a 97% follow-up rate at six weeks [4].
Provider support plays a key role in encouraging app adoption. While rural residents are less familiar with digital mental health tools (21% compared to 16% in non-rural areas), recommendations from healthcare providers can significantly boost acceptance [2].
Cost-Effectiveness and Accessibility
Mobile health apps aren’t just clinically effective – they’re also budget-friendly. Traditional therapy can be costly and hard to access for rural populations. Apps offer a scalable, lower-cost alternative. Prescription Digital Therapeutics (PDTs), for example, are software-based treatments prescribed by providers that allow for continuous monitoring and progress tracking between appointments. By reducing the need for in-person visits, these tools can help cut treatment costs [2].
The financial benefits extend to healthcare institutions as well. Digital interventions can lower annual nurse turnover costs from $16,736 per nurse to $11,592 – a savings of over $5,000 per individual [3]. This scalability makes mental health support more attainable, even in areas with limited resources.
"Digital therapeutics provide a scalable approach to bridging this gap… overcoming barriers of geography, stigma, and limited specialist availability." – Alejandro López-Tello, Universidad Iberoamericana [1]
A survey found that 89% of rural respondents believe PDTs can address at least one major barrier to care [2]. By delivering professional-grade therapy through software, these tools offer a lifeline to communities that traditional mental health care models have overlooked. For rural areas grappling with chronic provider shortages, mobile health apps are more than a convenience – they’re a necessity.
Research Findings and Real-World Examples
Patient Engagement and Outcomes
Mobile mental health apps show measurable success, especially when users actively engage with them. For instance, between March and October 2024, researchers in Mexico tested Aurora, a Spanish-language CBT app developed by Psicofarma S.A. de C.V., with adults experiencing mild-to-moderate anxiety or depression. The results were striking: participants who completed six or seven modules saw anxiety decrease by 3.9 points and depression by 4.0 points. On the other hand, those with minimal engagement (zero to two modules) experienced much smaller reductions – 0.9 points for anxiety and 1.0 points for depression [1]. The takeaway? Higher engagement leads to better outcomes.
The RESiLIENT trial in Japan, conducted from September 2022 to February 2024, echoed these findings on a broader scale. Involving 3,936 adults with subthreshold depression, the trial tested a smartphone app offering five CBT techniques: behavioral activation, cognitive restructuring, problem-solving, assertion training, and insomnia therapy. The results were impressive: 84% adherence and 97% follow-up at six weeks, a significant improvement over the usual 30% adherence rate for unguided internet programs [4]. Symptom reduction effect sizes ranged from -0.16 to -0.67, with benefits lasting up to 26 weeks [4].
These studies highlight the potential of digital tools to complement traditional care, setting the stage for hybrid care models.
Hybrid Models of Care
Hybrid care models combine mobile apps with clinical oversight, offering a promising solution for patients in rural areas. In the Aurora study, the app was used as a digital adjunct to pharmacotherapy, allowing patients to continue medication while working through CBT modules between psychiatrist visits [1]. This approach addresses a major challenge in rural areas, where 21% of patients struggle to manage their mental health between in-person appointments [2]. By integrating apps into care plans, these models help tackle issues like provider shortages and transportation barriers.
The role of healthcare providers in encouraging app adoption is critical. While rural populations may be less familiar with digital mental health tools, 97% of patients said they would use a digital therapeutic if recommended by their doctor [2]. This aligns with the Prescription Digital Therapeutic (PDT) model, where clinicians formally prescribe apps. A 2024-2025 survey found that 89% of rural respondents believed PDTs could address at least one major barrier to care [2].
AI tools further enhance hybrid care by automating tasks like triage and reminders, freeing up clinicians to focus on complex cases. For example, AI chatbots have reduced anxiety symptoms by 60% in healthcare workers, while mindfulness apps have lowered perceived stress by 30% [3]. These tools don’t replace human care – they extend it, offering 24/7 support in areas where 65% of counties lack even a single psychiatrist [2].
Barriers to Adoption in Rural Settings
Technology Access and Digital Literacy
Mobile mental health apps face uphill battles in rural America, primarily due to infrastructure gaps. Many rural areas lack reliable broadband, making it tough to use apps that rely on cloud services or telemedicine [2][3]. On top of that, not everyone in these regions has access to the necessary devices, deepening the "digital divide" [3]. For example, only 55% of rural residents track their health digitally, compared to 73% in non-rural areas. Additionally, 21% of rural residents are unfamiliar with digital mental health apps altogether [2].
A study of the Aurora app, conducted from March to October 2024, highlighted these challenges. While 81.6% of participants reported psychological improvements, many struggled with the app’s limited offline capabilities and its dependence on constant internet access [1]. These connectivity issues make it harder for rural users to adopt and consistently engage with such tools.
User Trust and Privacy Concerns
Technical issues aside, trust plays a major role in whether rural users stick with digital mental health tools. In these communities, trust often hinges on recommendations from healthcare providers. A staggering 97% of rural respondents said they’d be more likely to use a digital therapeutic if their provider endorsed it [2].
Privacy is another sticking point. In tight-knit rural communities, people may worry about being recognized when seeking help, which can discourage them from using mental health therapy services. Apps can address this by emphasizing strong privacy protections and clear data policies. Prescription Digital Therapeutics, which require FDA approval, clinical trial validation, and a physician’s prescription, are another way to build trust. These regulatory measures reassure users about safety and effectiveness [2].
Long-Term User Retention
Keeping rural users engaged over time is another hurdle. Only 28% of rural users interact with health apps daily, compared to 41% of urban and suburban users [2]. Yet, studies show that consistent engagement leads to better outcomes. Simplifying app interfaces could be key to improving retention rates [1].
Unfortunately, many apps feature overly complicated designs, which drive abandonment rates as high as 70–80% [3]. Educational gaps add to the problem – only 12% of rural residents hold a bachelor’s degree or higher, compared to 28% in non-rural areas [2]. By creating simpler, more intuitive designs with less text and lower cognitive demands, developers could make these tools more accessible and appealing to rural users. Tackling these retention challenges is just as critical as addressing geographic and financial barriers.
Research Gaps and Future Directions
Long-Term Efficacy and Safety Studies
Most studies in this field wrap up within weeks, leaving many unanswered questions about the long-term effects. For example, the RESiLIENT Randomized Controlled Trial (2022–2024) followed 3,936 adults with subthreshold depression for 26 weeks, achieving an impressive 97% follow-up rate at week six. The study found that therapeutic benefits persisted even with reduced app usage after 10 weeks [4].
However, safety remains a major concern. AI-powered chatbots often fail to detect suicidal tendencies or pick up on subtle emotional cues [5][6]. Research from Stanford highlights another issue: these systems tend to show more stigma toward conditions like alcohol dependence and schizophrenia compared to depression [6]. Nick Haber, Assistant Professor at Stanford Graduate School of Education, summed up the risks:
"LLM-based systems are being used as companions, confidants, and therapists… But we find significant risks, and I think it’s important to lay out the more safety-critical aspects of therapy" [6].
To mitigate these risks, experts suggest hybrid care models that combine digital tools with human oversight for crisis management [5][3]. These findings emphasize the importance of conducting more extensive, long-term research to ensure safety and sustained effectiveness in digital mental health solutions.
Standardizing Effectiveness Metrics
One of the biggest challenges in the mental health app space is the lack of consistent ways to measure success. Many studies rely on basic metrics like log-in counts, which don’t truly reflect the impact of these interventions. For instance, trials like Aurora have demonstrated measurable dose-response effects, showing a need for more robust evaluation methods [1].
Researchers are now pushing for master protocols that test various app components against shared controls. This approach could help identify which features – such as behavioral activation or cognitive restructuring – actually lead to meaningful improvements. However, the "Dodo bird verdict" complicates matters, suggesting that without dismantling studies, all therapies might appear equally effective [3][4]. Tools like the System Usability Scale and validated symptom scales like PHQ-9 offer a starting point for measuring outcomes. Still, these tools need to be re-evaluated for use in rural and diverse populations [1][3]. Developing standardized metrics is critical to ensure these tools work effectively in resource-limited settings.
Serving Underrepresented Populations
Inclusivity is another pressing issue. For rural users, addressing digital literacy gaps and creating culturally relevant designs is essential. Research on mental health apps has largely overlooked key groups, such as older adults and culturally diverse populations. A promising example of inclusive design comes from the Aurora app study. Led by Edith Zárate and Oscar Arias-Carrión between March and October 2024, this project used a co-creation framework involving 20 clinicians and 12 psychiatric patients to develop a Spanish-language CBT app. This approach highlights how inclusive design can better serve underrepresented groups [1].
Bridging digital literacy gaps through training and subsidized devices is equally important. Currently, only 12% of rural residents have a bachelor’s degree or higher, compared to 28% in non-rural areas [2]. Developers must also tackle algorithmic biases by adopting ethical AI practices [3]. Future research should move beyond short-term studies to assess how these tools perform across diverse age groups, languages, and cultural contexts over longer periods, such as 6–12 months [1][3].
Conclusion
Mobile health apps hold the potential to reshape rural mental health care, especially in areas grappling with severe provider shortages and geographic challenges [2]. These apps offer around-the-clock support, eliminate the need for travel, and make evidence-based treatments like Cognitive Behavioral Therapy (CBT) more accessible and affordable compared to traditional methods.
Research highlights significant reductions in mental health symptoms among users who actively engage with these tools [1]. Interestingly, most patients are willing to use digital therapeutics when recommended by their providers, even though awareness of these technologies remains relatively low [2].
However, to fully realize the benefits of these tools, critical challenges must be addressed. Future research should focus on validating their long-term safety and creating standardized metrics for evaluation. Additionally, expanding broadband access, offering digital literacy programs, and involving rural communities in the design process are vital steps toward ensuring fair and effective implementation [2][3]. Hybrid care models that blend therapy AI solutions with human oversight and culturally tailored approaches for underserved populations provide a promising path forward.
For rural areas burdened by provider shortages, isolation, and stigma, these digital solutions offer a lifeline to much-needed care. By focusing on scalable and community-centered approaches, these tools can pave the way for a brighter future in mental health care.
FAQs
Do mental health apps work as well as therapy?
Mental health apps have proven to be a helpful resource, particularly for individuals who face challenges accessing in-person care, such as those living in rural areas. Many of these apps incorporate evidence-based methods like cognitive behavioral therapy (CBT) to assist users in managing symptoms of depression, anxiety, and stress. That said, these tools are typically viewed as complements to traditional therapy rather than replacements. While they can provide accessible and convenient support, they often lack the tailored, in-depth care that only a trained therapist can provide.
What if my internet is too slow for a mental health app?
A sluggish internet connection can make it tough for people, especially in rural areas, to access digital mental health tools. To tackle this issue, some apps have introduced features like offline access, low-bandwidth modes, and asynchronous communication. Additionally, hybrid models that blend digital tools with in-person support are stepping in to fill the gap. These approaches are designed to help users in areas with spotty internet connectivity still benefit from mental health resources.
How private is my data in a mental health app?
Data privacy is a top priority when it comes to mental health apps because they handle some of the most sensitive personal information. Trusted apps, such as Aidx.ai, take privacy seriously by implementing measures like encryption, adhering to GDPR regulations, and even providing features like optional incognito modes for added discretion. That said, privacy standards can differ widely between apps. Always take the time to review an app’s privacy policies to ensure your data is protected and won’t be shared without your consent.